Recent reporting of residents queueing for hours outside new NHS dental practices – a visible sign of the growing struggle to access routine dental care – echoes the national patterns previously identified in research by Dr Stephen Clark.
These real‑world experiences, together with emerging evidence, highlight a system facing significant spatial inequalities, with some places effectively becoming ‘dental deserts’ while others retain only modest provision.
Ahead of the NHS dentistry quality and payment reforms next month, we’re looking back at Stephen’s research in the European Journal of Public Health which revealed the places across England where NHS dental provision is under the greatest pressure and where unmet need is most acute.
The problem
As part of the National Health Service (NHS) residents in England have the right to visit a dentist for twice yearly check-ups and treatment. However access to this care is proving to be increasingly difficult.
The mainstream media regularly contains stories of individuals who are unable to get an appointment, have to make visits to A&E departments, travel 100’s of miles to find a dentist, carry out DIY treatments, or return to war zones for dental treatment.
This is a bad situation because poor dental health can have both physical and psychological impacts on people’s quality of life and without check-ups opportunities to detect more serious illness, e.g. mouth cancer, are lost.
How is NHS dentistry provided in England?
Within England a dentist can agree to work to an NHS contract.
If they do then they will be contracted to deliver a set number of Units of Dental Activity (UDA) throughout the year and paid an amount of money per UDA by the government.
Almost all NHS care is allocated to one of three bands and there is a set fee for each band, payable by the patient.
| Band | Example Care/Treatments | NHS patient cost (2026) | UDAs |
| Band 1 | Check-up; X-ray; Light polish | £27.90 | 1 |
| Band 2a to 2c | Filling; Extraction; Deep de-scaling | £76.60 | 3, 5 or 7 |
| Band 3 | Crowns; Dentures; Bridges | £332.10 | 12 |
| Urgent or Unscheduled Care | £75.00 | 1.2 |
The patient pays the same irrespective of the number of teeth treated and only pays the highest fee appropriate, so an examination followed by some form of band 2 treatment costs just the band 2 fee, £76.60.
From April 2026 practices are expected to allocate 8.2% of their contract value to providing urgent or unscheduled care. Also new UDA changes will provide patients with very high needs access to new care packages that pay dental professionals a higher rate than previously.
Looking at the population, back in 2023-2023 when this study was conducted, there was the equivalent of 1.6 contracted UDAs per person available, which is less than is required to carry out twice yearly check-ups and does not allow any capacity for treatments.
Improving understanding of NHS dentistry provision through research
It is at this point that Stephen’s research becomes relevant. It answers the questions as to where is the NHS provision currently poor?; and what will be the overall impact of adding potential extra NHS capacity be in certain communities?
This is done by using a measure of accessibility.
An accessibility index measure should have the features that it should increase as:
- the number of supply locations or care capacity increases
- there is a lower amount of demand and competition
- there is a reduction in the distance between patients and practices
An additional requirement is that there should be no detriment in dental care accessibility by the type of community.
In this study the demand for NHS dentistry is the 2021 Census population in the Lower Super Output Area (LSOA) (each has a population of about 1,600), the supply of NHS dentistry is the number of UDAs contracted to the practice, and the distance is the travel time by car between the LSOA population weighted centroid and the practice location postcode.
The calculations are made using the Modified Huff Variable 3 Stage Floating Catchment Area (MHV3SFA) approach.
This index of accessibility incorporates all the features that are highlighted above. In the calculations, an area with better accessibility to NHS care (more practices; little local competition for the care; or being close by) will have a higher index than one with poorer access (fewer practices; high local demand for care; or long travel times).
The details of this calculation can be found in the accompanying article.
Dental deserts
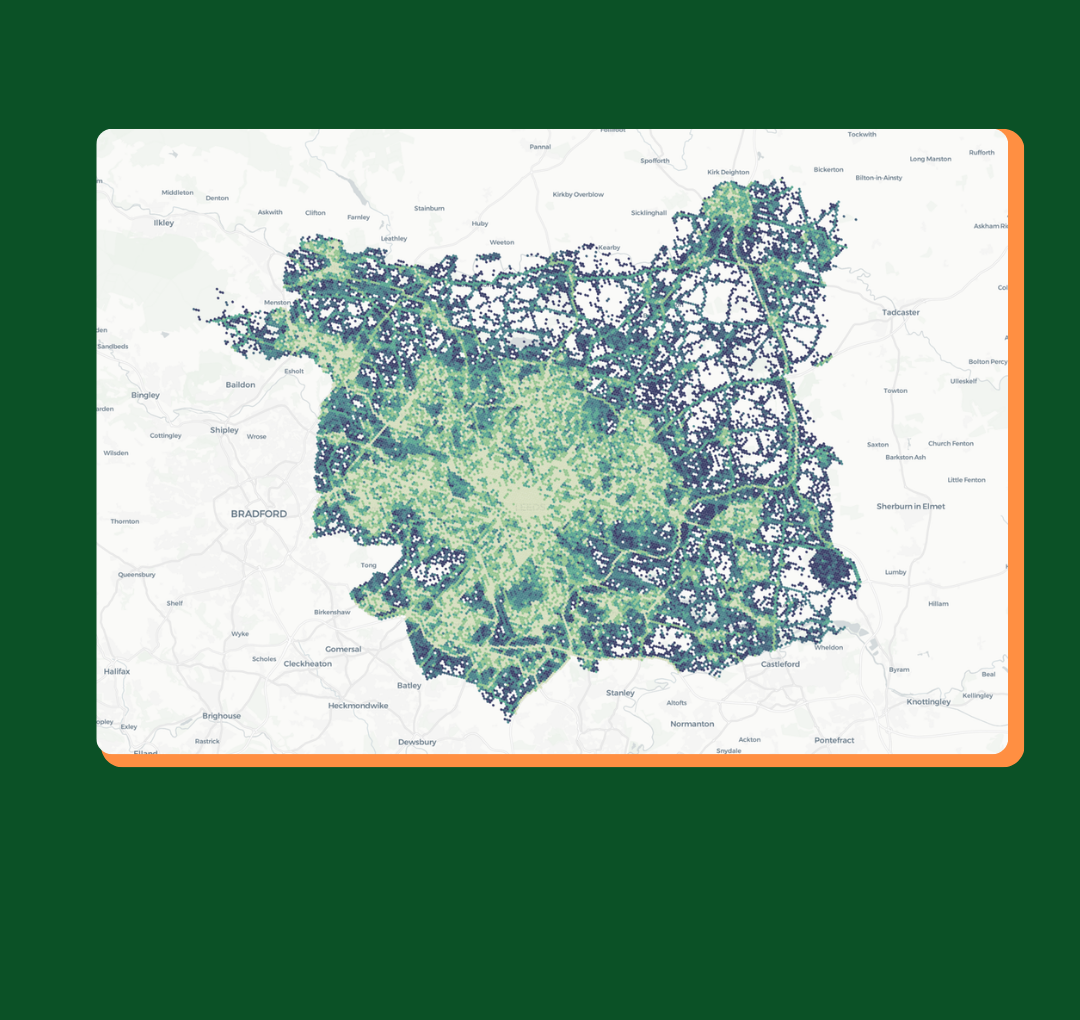
The figure below maps the accessibility index for the LSOAs in England. The areas with better accessibility and a higher index are in lighter shades, the areas with poorer accessibility are in darker shades. Additionally the 1% of LSOAs with the lowest accessibility are highlighted with a blue diamond and could be considered ‘dental deserts’. It is clear from this figure that urban areas have generally better accessibility to NHS dental care than the rural locations.

Figure 1 : Accessibility index for England
This figure identifies clusters of LSOAs that could be said to form dental deserts. Two are located in the East of England, in the Fenland and Mid Suffolk, others in the South Midlands and along the Welsh border, and finally in the South West.
If we zoom into the situation in the Fenlands as shown in Figure 2, we see some interesting features. Although the town of Wisbech in the centre of the figure has two dental practices, they are only contracted to provide 36,000 UDAs as part of their NHS contract. This means that some very close by neighbourhoods have a reasonable level of accessibility but others, shown in red here, are still close by but have very poor accessibility.
The areas around the towns of Wisbech and March would be a top priority for extra NHS dental capacity. The MHV3SFA calculations could then be repeated with this extra capacity, and its impact on the accessibility for these LSOA could be evaluated.
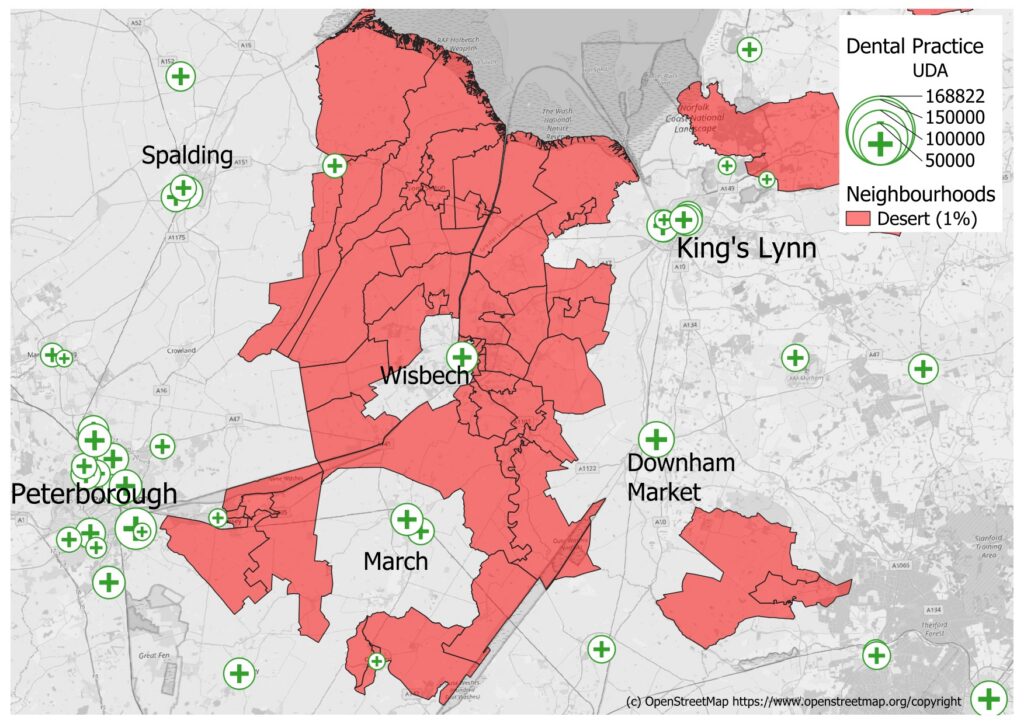
Figure 2 The dental desert in the Fenlands
In the article a similar case study is presented for the St Pauls community in Bristol. Also the article profiles accessibility by various measure of deprivation and rurality. The more deprived and urban neighbourhoods have better accessibility than affluent and rural communities.
Extra NHS dentistry capacity should be targeted in the right locations
The level of provision of NHS dentistry is a known problem. But the problem is spatially variable. There are some locations lucky to have modest provision whilst others could be considered deserts. If this situation is to change it is important that any extra capacity for care is targeted in the right locations – where it is needed.
Ten areas that should be be a top priority for NHS dentistry investment (in alphabetical order):
- Eye – Mid Suffolk
- Kington – Herefordshire
- Launceston – Cornwall
- Leyburn – Richondshire
- Malton – Ryedale
- Millom – Copeland
- Padstow – Cornwall
- Stow-on-the-Wold – Cotswold
- Tisbury – Wiltshire
- Wisbech – Fenland
The level of provision of NHS dentistry is a known problem. But both availability and accessibility vary by location and by the characteristics of the neighbourhood.
Further Information
Read the paper in full: Spatial Disparities in Access to NHS Dentistry: A Neighbourhood-Level Analysis in England
Dr Clark has also had a companion piece published in the British Dental Journal on the recent trends in availability of NHS dental care and how this varies by the characteristics of the neighbourhood.
Dr Stephen Clark is a Research Fellow at the Healthy and Sustainable Places Data Service at the University of Leeds.